Quality of Life and Health Behaviors
The World Health Organization (WHO) defines quality of life as ‘a broad ranging concept affected in a complex way by the person’s physical health, psychological state, level of independence, social relationships and their relationship to the salient features in their environment’. Quality of life and health behaviors are interconnected.
Quality of life refers to the degree of excellence people appraise their lives to contain. However, people around the world appraise excellence with similar criteria, such as performing daily activities, energy or discomfort, positive and negative feelings, personal control, interpersonal relations, pleasant activities, personal and intellectual growth, and material possessions.
Quality of life has several components—
- Physical functioning,
- Psychological status,
- Social functioning, and
- Disease or treatment related symptoms.
Researchers focus on how much the disease and its treatment interfere with the activities of daily living. Such as sleeping, eating, going to work, and engaging in recreational activities. Essentially, then, quality-of-life assessments gauge the extent to which a patient’s normal life activities have been compromised by disease and treatment. A broad array of measures is available for evaluating quality of life in both adults and children (Varni, Burwinkle, Rapoff, Kamps, & Olson, 2004).

Quality of Life Components (NHS)
Furthermore, quality-of-life information can inform practitioners about care that will maximize long-term survival with the highest quality of life possible (Kaplan, 2003).
Health Promotion
Health promotion is a philosophy that has at its core the idea that good health, or wellness. It is a personal and collective achievement. For the individual, it involves developing a program of good health habits. Health promotion and health education perspectives tend to emphasize the role of knowledge in predicting health behaviors and aim to change behaviors by improving what people know.
For the health psychologist, health promotion involves the development of interventions to help people practice healthy behaviors. For the medical practitioner, health promotion involves teaching people how to achieve a healthy lifestyle. And also helping people at risk for particular health problems off set or monitor those risks.
Health Behaviour and Healthy Habits
Health behaviors are behaviors that people undertake to enhance or maintain their health. They are important in predicting mortality and the longevity of individuals. A health habit refers to firmly established health behaviors and often performed automatically, without awareness.
These habits usually develop in childhood and begin to stabilize around age 11 or 12 (Cohen, Brownell, & Felix, 1990). Wearing a seat belt, brushing one’s teeth, and eating a healthy diet are examples of these kinds of behaviors. Although a health habit may develop initially because positive outcomes reinforce it, such as parental approval, it eventually becomes independent of the reinforcement process.
For example, you may brush your teeth automatically before going to bed. As such, habits can be highly resistant to change. Consequently, it is important to establish good health behaviors and to eliminate poor ones early in life.
Some important 7 health behaviors-
- Sleeping 7 to 8 hours a night
- Not smoking
- Eating breakfast each day
- Having no more than one or two alcoholic drinks each day
- Getting regular exercise
- Not eating between meals
- Being no more than 10 percent overweight
Primary Prevention Instilling good health habits and changing poor ones is the task of primary prevention. This means taking measures to combat risk factors for illness before an illness has a chance to develop. There are two general strategies of primary prevention. The first and most common strategy is to get people to alter their problematic health behaviors, such as helping people lose weight through an intervention. The second, more recent approach is to keep people from developing poor health habits in the first place.
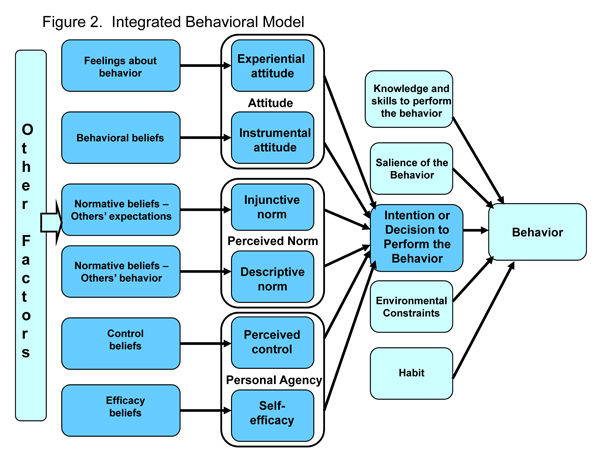
Integrated Behavior Change Model
Factor Affecting Health Behaviors
- Demographic Factors – Younger, wealthy, better-educated people with less stress and high social support typically practice better health habits than people with high stress & fewer resources (Hanson & Chen, 2007).
- Age – Health habits are typically good in childhood, deteriorate in adolescence and young adulthood, but improve again among older people.
- Values – Values affect the practice of health habits. For example, exercise for women may be considered desirable in one culture but undesirable in another (Guilamo-Ramos, Jaccard, Pena, & Goldberg, 2005).
- Personal Control – People who regard their health as under their personal control practice better health habits than people who regard their health as due to chance. However, the health locus of control scale (Wallston, Wallston, & DeVellis, 1978) measures the degree to which people perceive their health to be under personal control, control by the health practitioner, or chance.
- Social Influence – Family, friends, and workplace companions influence health-related behaviors, sometimes in a beneficial direction, other times in an adverse direction (Broman, 1993; Turbin et al., 2006). For example, peer pressure often leads to smoking in adolescence but may influence people to stop smoking in adulthood. However, personal Goals and Values Health habits are tied to personal goals. If personal fitness is an important goal, a person is more likely to exercise.
- Perceived Symptoms –Perceived symptoms control some health habits. For example, a smoker who wakes up with a smoker’s cough and raspy throat may cut back in the belief that he or she is vulnerable to health problems at that time.
- Access to the Health Care Delivery System – Access to the health care delivery system affects health behaviors. For example, obtaining a regular Pap smear, getting mammograms, and receiving immunizations for childhood diseases depend on access to health care. the health care system through lifestyle advice indirectly encourages other behaviors, such as losing weight and stopping smoking,
- Knowledge and Intelligence – The practice of health behaviors is tied to cognitive factors, such as knowledge and intelligence (Jaccard, Dodge, & Guilamo-Ramos, 2005). However, more knowledgeable and smarter people typically take better care of themselves. Also, people who are identified as intelligent in childhood have better health-related biological profiles in adulthood, which may be explained by their practice of better health behaviors in early life (Calvin, Batty, Lowe, & Deary, 2011).

Determinants of Health
Read More- How to Change Health Habits?
References
Ogden, J. (2017). Health psychology: A textbook (4th Ed.).McGraw Hill Education.
Taylor, Shelley E. (2018). Health Psychology (10th Ed). McGraw Hill Higher Education. Indian Edition.
Niwlikar, B. A. (2022, March 23). Quality of life and Health Behaviors- 8 Factors That Influence Them. Careershodh. https://www.careershodh.com/quality-of-life-and-health-behaviors/
